Contents:
- What is cerebrovascular disease
- Which conditions belong to CVD
- What triggers the development of CVD
- Cerebrovascular disease: symptoms and stages of development
- Possible complications of cerebrovascular diseases
- How to diagnose cerebrovascular diseases
- How cerebrovascular diseases are treated
Disorders of blood circulation in the vessels of the brain can develop gradually and remain almost unnoticed for a long time. A person may experience recurrent headache, dizziness, fatigue, or worsening concentration or memory, without linking these symptoms to vascular problems.
Such changes may be associated with the development of cerebrovascular diseases, which affect the blood supply to the brain and the functioning of the nervous system. In some cases, disorders develop gradually, and sometimes they may present as acute conditions.
In this article, we will discuss what cerebrovascular diseases are, which conditions belong to them, what symptoms may indicate a problem, and how diagnosis and treatment are carried out.
What is cerebrovascular disease
Cerebrovascular diseases (CVD) are a collective term for a group of diseases and conditions associated with impaired blood circulation in the vessels of the brain. They occur when the blood supply to brain tissues decreases or stops due to vascular damage.
The brain needs a constant supply of oxygen and nutrients through the blood. Even a slight reduction in blood flow can affect the functioning of nerve cells, and prolonged impairment of blood circulation can lead to their damage.
The most common causes of such changes are narrowing or blockage of blood vessels, formation of blood clots, as well as structural damage to the vessel wall. As a result, the nourishment of brain tissues worsens and various neurological symptoms occur.
Cerebrovascular diseases can have different courses. In many cases, disorders develop gradually and manifest as chronic deterioration of cerebral blood circulation. At the same time, sometimes they occur suddenly and lead to acute conditions that require urgent medical care. That is why early detection of changes in the vessels of the brain is important for preventing serious complications.
Which conditions belong to CVD
Cerebrovascular diseases include various conditions that arise due to impaired blood circulation in the vessels of the brain. They can have both a chronic and an acute course. In most cases, changes in blood vessels form gradually, but sometimes impaired circulation occurs suddenly and leads to urgent conditions.
Depending on the course, two main groups of cerebrovascular disorders are distinguished.
Chronic disorders of cerebral blood circulation:
- chronic cerebral ischemia — a gradual decrease in the blood supply to brain tissues;
- discirculatory encephalopathy — brain damage associated with prolonged impairment of blood circulation;
- vascular dementia — deterioration of memory, thinking, and other cognitive functions due to damage to brain vessels.
Acute disorders of cerebral blood circulation:
- transient ischemic attack — a short-term impairment of cerebral blood circulation in which neurological symptoms usually resolve within 24 hours;
- ischemic stroke — occurs due to blockage of a cerebral artery by a blood clot or an atherosclerotic plaque;
- hemorrhagic stroke — associated with rupture of a blood vessel and bleeding into brain tissue.
These conditions have different mechanisms of development, however, all of them are associated with impaired blood supply to the brain and can lead to neurological symptoms of varying severity. That is why it is important to consult a doctor in a timely manner when the first signs of impaired cerebral blood circulation appear.
What triggers the development of CVD
Most often, cerebrovascular diseases develop against the background of changes in blood vessels or under the influence of factors that reduce blood flow and increase the risk of blood clot formation.
Doctors at “Oxford Medical” note that one of the most common causes is atherosclerosis. In this case, atherosclerotic plaques form on the walls of arteries, narrowing the vessel lumen and reducing blood flow to the brain. If a plaque significantly blocks a vessel or causes a blood clot to form, this can lead to an acute disorder of cerebral blood circulation.
Arterial hypertension also plays an important role. Persistently elevated blood pressure gradually damages the walls of blood vessels, making them less elastic and more vulnerable to injury.
Factors that may contribute to the development of cerebrovascular disorders include:
- vascular atherosclerosis;
- high blood pressure;
- diabetes mellitus;
- elevated cholesterol levels;
- obesity;
- a sedentary lifestyle;
- smoking;
- chronic stress.
In addition, the risk of disorders of cerebral blood circulation may increase with other diseases of the cardiovascular system. For example, in people who have developed coronary heart disease, systemic vascular changes are often observed, which can also affect the blood supply to the brain.
The likelihood of developing cerebrovascular diseases also increases with age. Gradual aging of blood vessels, combined with the action of risk factors, can lead to changes in their structure and impairment of normal blood circulation.
Cerebrovascular disease: symptoms and stages of development
Manifestations of impaired cerebral blood circulation may differ depending on the type of vascular damage, the rate of changes, and the degree of impairment of the blood supply to the brain. In many cases, cerebrovascular disorders develop gradually, but sometimes they may present as sudden acute conditions.
The most common symptoms include:
- headache;
- dizziness;
- ringing in the ears;
- rapid fatigue;
- memory impairment;
- difficulty concentrating;
- impaired coordination of movements;
- unsteadiness when walking;
- numbness or weakness in the limbs.
With chronic disorders of cerebral blood circulation, symptoms usually worsen gradually. At first, a person may experience recurrent headache, fatigue, and difficulty concentrating. Over time, more pronounced cognitive impairment, unsteadiness when walking, and memory impairment may appear.
At the same time, some cerebrovascular pathologies can develop suddenly. For example, in stroke the following symptoms occur:
- sudden weakness or numbness of an arm or leg;
- facial asymmetry;
- speech impairment;
- sudden dizziness or impaired coordination.
In such cases, it is necessary to seek medical help immediately.
Possible complications of cerebrovascular diseases
.jpg)
If impaired blood circulation in the vessels of the brain progresses or remains untreated for a long time, this can lead to serious complications. The most dangerous of these is stroke — an acute disorder of cerebral blood circulation.
Stroke occurs when an area of the brain suddenly stops receiving an adequate blood supply. This may happen because a blood vessel is blocked by a clot or because it ruptures and bleeding occurs into brain tissue. In such a situation, some nerve cells are damaged or die, which can lead to various disorders of the nervous system.
After a stroke or prolonged impairment of the blood supply to the brain, the following consequences may occur:
- weakness or paralysis of the limbs — reduced strength in an arm or leg, more often on one side of the body;
- speech impairment — a person may find it difficult to speak, pronounce words, or understand the speech of others;
- impaired coordination and balance, unsteadiness when walking;
- memory and concentration impairment;
- reduced sensation in certain areas of the body;
- gradual worsening of thinking and memory, which in medicine is called vascular dementia.
Such complications can significantly affect a person’s daily life, their ability to work, move, or perform routine tasks. That is why, when symptoms of impaired cerebral blood circulation appear, it is important to consult a doctor in a timely manner and undergo the necessary examinations. Early diagnosis helps reduce the risk of severe consequences.
How to diagnose cerebrovascular diseases
When symptoms of impaired cerebral blood circulation appear, the first step is to consult a neurologist. This specialist is responsible for diagnosing cerebrovascular diseases, assessing neurological status, and determining the further examination plan.
During the consultation, the doctor analyzes the patient’s complaints, the duration and nature of symptoms, and the presence of risk factors — high blood pressure, diabetes mellitus, and cardiovascular diseases. A neurological examination is also performed to assess strength in the limbs, coordination of movements, sensation, speech, memory, and other functions of the nervous system.
To уточнения диагноза могут назначаться инструментальные исследования:
- ultrasound examination of the vessels of the neck and head — makes it possible to assess the condition of the carotid and vertebral arteries, detect their narrowing or impaired blood flow;
- computed tomography — used mainly when acute cerebral circulation impairment is suspected;
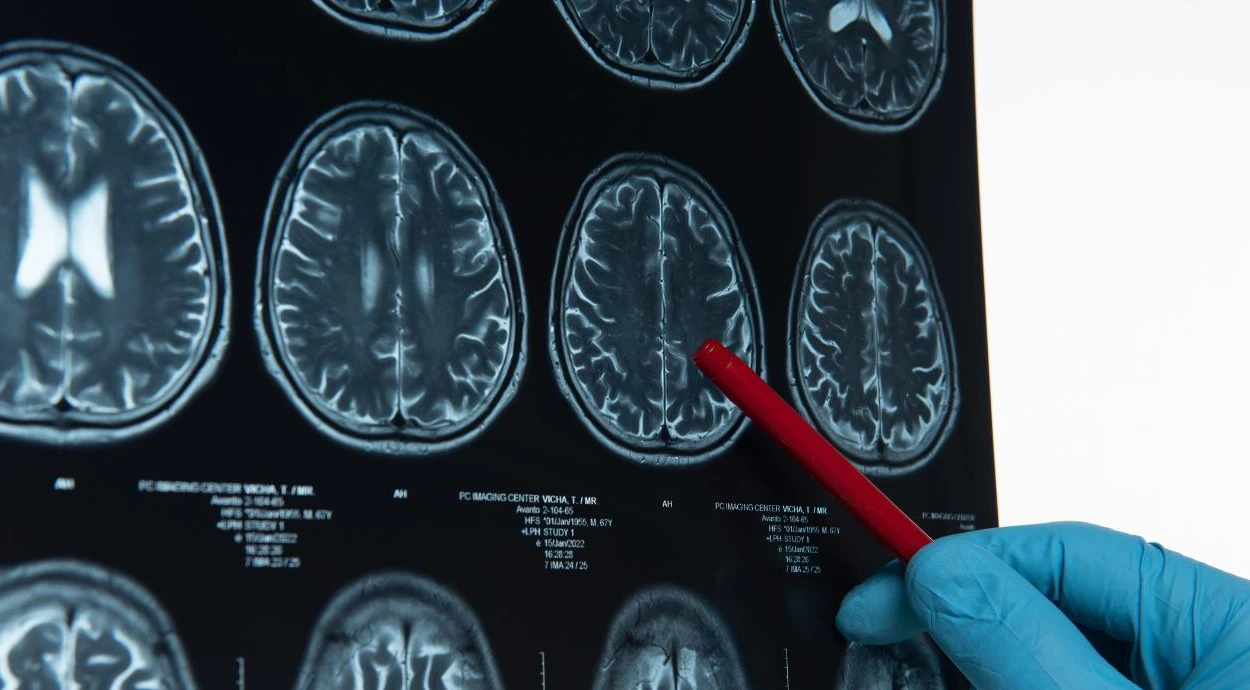
- magnetic resonance imaging — makes it possible to assess the structure of brain tissue in detail and detect areas of ischemia or other changes;
- laboratory blood tests — help determine glucose, cholesterol levels, and other indicators that affect the condition of blood vessels.
If needed, angiography may be performed — a vascular imaging study in which a contrast agent is injected into the bloodstream and X-ray equipment is used to obtain images of blood vessels. This method allows the site of narrowing, blockage, or vascular abnormalities to be seen and the degree of impaired blood flow to be assessed.
If a significant narrowing of the major arteries is detected during the examination, the neurologist may refer the patient to a consultation with a vascular surgeon to assess the need for surgical intervention. If there are concomitant heart diseases, a cardiologist consultation may be required.
A comprehensive diagnostic approach makes it possible not only to confirm the presence of a cerebrovascular disease, but also to determine the cause of impaired circulation and choose the optimal treatment strategy.
How cerebrovascular diseases are treated
Treatment of cerebrovascular diseases is aimed at stabilizing cerebral blood circulation, preventing thrombosis, and reducing the risk of stroke. The treatment strategy depends on the cause of the disorder, the extent of vascular damage, the nature of symptoms, and the presence of concomitant diseases.
In most cases, treatment is комплексным and combines медикаментозную therapy, control of risk factors, and, if necessary, surgical or endovascular methods.
The main directions of treatment include:
- Drug therapy. The doctor may prescribe medications to reduce the risk of blood clot formation, control blood pressure, correct cholesterol levels, and treat concomitant cardiovascular diseases. The treatment regimen is selected individually, taking into account the clinical situation.
- Blood pressure control. Arterial hypertension is one of the key risk factors for cerebral vascular damage. Selecting antihypertensive therapy helps reduce the load on the vascular wall and reduce the risk of stroke.
- Correction of cholesterol and glucose levels. Elevated cholesterol contributes to the formation of atherosclerotic plaques, and diabetes mellitus accelerates vascular damage. Controlling these indicators is an обязательной component of complication prevention.
- Lifestyle changes. Smoking cessation, weight normalization, regular physical activity, and рациональное diet are recommended. This helps slow the progression of vascular changes.
- Surgical or endovascular treatment. In cases of significant narrowing of major arteries that supply blood to the brain, surgery may be performed. In such cases, treatment is provided by a vascular surgeon who performs operations or endovascular procedures to restore vessel patency and reduce the risk of stroke.
If a cerebrovascular disease presents as an acute impairment of cerebral blood circulation, treatment is carried out in a specialized hospital and requires urgent medical care.
Timely treatment and control of risk factors help slow the progression of the disease and significantly reduce the likelihood of stroke and other severe consequences.
The information in this article is provided for informational purposes only and is not a guide to self-diagnosis or treatment. If symptoms of the disease appear, you should consult a doctor.
Sources:
European Stroke Organisation (ESO)
National Institute of Neurological Disorders and Stroke (NINDS, NIH)