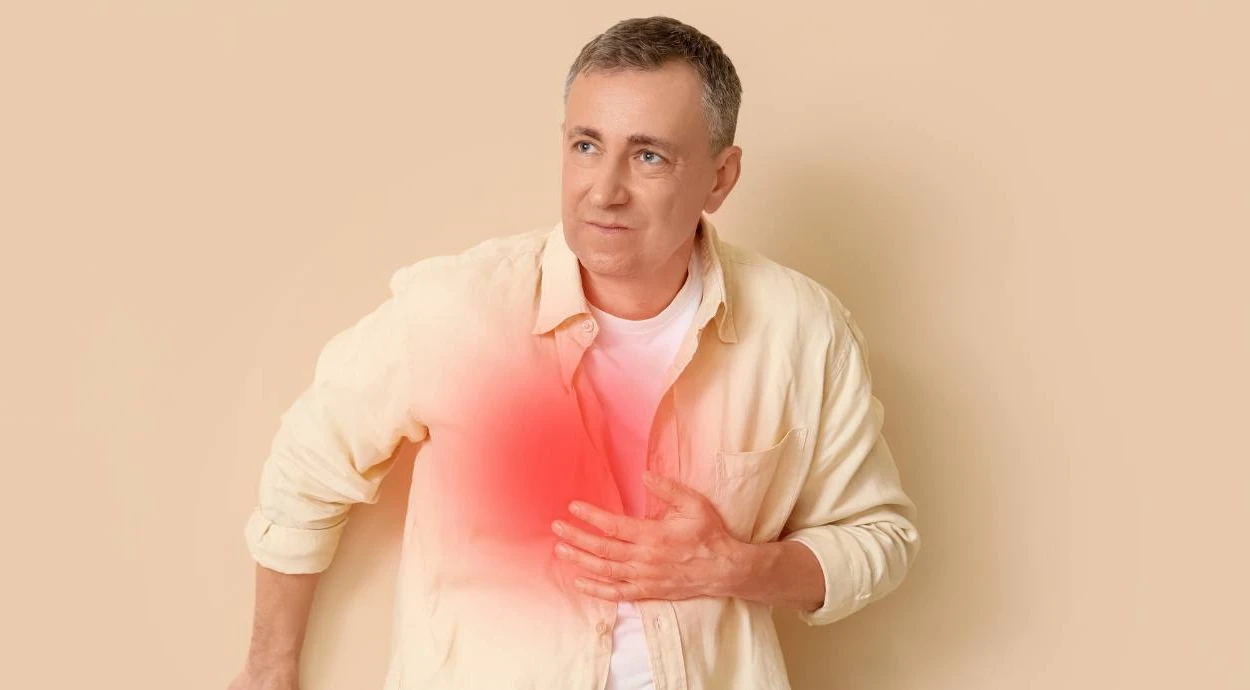
Myocardial infarction is a dangerous condition in which a part of the heart muscle stops receiving enough blood and oxygen. In such a situation, every minute counts, because without timely medical care, heart damage can become irreversible and life-threatening.
The problem is that a heart attack does not always begin suddenly and obviously. Chest discomfort, shortness of breath, weakness, or an unexplained deterioration in well-being are often ignored or attributed to fatigue, stress, or other causes. As a result, seeking medical help is delayed, and the risk of complications increases.
In this article, we will explain step by step how a heart attack begins, what signs may occur, what to do if a heart attack is suspected, and how to reduce the risk of its development.
What Is a Heart Attack
A myocardial infarction is a condition in which a part of the heart muscle is damaged due to a sudden disruption of blood flow. Most often, this occurs when one of the coronary arteries that supply blood to the heart suddenly narrows or becomes completely blocked. As a result, myocardial cells do not receive oxygen and nutrients and begin to die.
Unlike temporary circulatory disorders, the changes in the heart caused by a heart attack are irreversible. The affected area of the muscle is gradually replaced by scar tissue that is unable to contract. Because of this, the heart begins to work less efficiently, which can affect blood supply throughout the body.
A heart attack is an acute cardiovascular condition and requires immediate treatment. The faster blood flow is restored in the damaged vessel, the smaller the extent of myocardial injury and the lower the risk of serious complications. That is why it is so important to understand what happens in the heart during an attack and not delay medical assistance.
What Is the Main Cause of Myocardial Infarction
The main cause is a sudden disruption of blood supply to the heart muscle. Most often, this occurs due to damage to the coronary arteries — the vessels that deliver oxygen and nutrients to the myocardium. When blood flow is sharply reduced or stops, heart cells begin to die.
The main causes of heart attack development include:
-
atherosclerosis of the coronary arteries, in which cholesterol plaques gradually narrow the vessel lumen;
-
rupture of an atherosclerotic plaque followed by the formation of a thrombus that blocks the artery;
-
thrombosis of the coronary vessels against the background of blood clotting disorders;
-
a sudden spasm of the coronary arteries, particularly during severe stress or hormonal changes;
-
increased strain on the heart in cases of hypertension or heavy physical overexertion;
-
complications of coronary heart disease.
In most cases, a heart attack does not occur suddenly in an otherwise healthy person. It is preceded by long-term changes in the vessels that may not cause obvious symptoms. That is why controlling cholesterol levels, blood pressure, and timely treatment of cardiovascular diseases are crucial for reducing the risk of a heart attack.
How a Heart Attack Begins
As a rule, the body sends warning signals even before the development of an acute attack, but these manifestations may be vague or atypical. That is why people often do not associate a deterioration in well-being with heart problems and postpone seeing a doctor.
In many patients, warning signs of a heart attack appear several days or hours before the attack. During this period, the heart muscle is already suffering from insufficient blood supply, but complete blockage of the vessel has not yet occurred. This pre-infarction condition requires special attention, as timely medical care can prevent severe heart damage.
Key manifestations from which a heart attack may begin include:
-
discomfort or pressure-like sensations in the chest that occur periodically;
-
shortness of breath during usual physical activity or even at rest;
-
a feeling of air hunger, inability to take a deep breath;
-
increased fatigue without an obvious reason;
-
dizziness, darkening of vision;
-
heart rhythm disturbances, a sensation of irregular heartbeats;
-
anxiety or an inner feeling of danger.
In some people, early symptoms may be mild or masked as other conditions — overwork, digestive problems, or the effects of stress. However, even minor but unusual changes in well-being related to the heart are a reason to consult a doctor, especially if they recur or gradually worsen.
Signs of a Heart Attack
The main signs include:
-
pain or pronounced discomfort in the chest;
-
a sensation of squeezing, pressure, or burning behind the breastbone;
-
shortness of breath, difficulty breathing;
-
sudden weakness, cold sweat;
-
heart rhythm disturbances;
-
dizziness or loss of consciousness;
-
anxiety, a feeling of fear.
Individual manifestations of a heart attack may vary in intensity, so below we will consider the most characteristic ones in more detail.
What Blood Pressure Is Typical During a Heart Attack
Blood pressure during a heart attack changes depending on the stage of the attack and the condition of the heart, but there are typical reference values to pay attention to. At the onset of a heart attack, many patients experience an increase in blood pressure to 150–180/90–110 mm Hg. This is associated with severe pain, fear, and the release of adrenaline.
As heart function worsens, blood pressure may drop sharply. A level below 90/60 mm Hg is considered dangerous, especially if it is accompanied by weakness, dizziness, or loss of consciousness. Such a drop in pressure indicates a serious circulatory disorder and requires immediate medical attention.
It is important to understand that normal or slightly altered blood pressure readings do not rule out a heart attack, so relying solely on numbers without evaluating other symptoms is dangerous.
What Pulse Is Typical During a Heart Attack
The pulse during a heart attack usually goes beyond normal limits. Most often, it is rapid — more than 90–100 beats per minute, sometimes reaching 120–130 beats or more. At the same time, the pulse may be irregular, with interruptions.
In some patients, especially when the heart’s conduction system is affected, the pulse may, on the contrary, slow down — fewer than 50–60 beats per minute. This condition is also dangerous and may be accompanied by dizziness or loss of consciousness.
Alarming signs include:
-
a sudden change in pulse rate;
-
an irregular rhythm;
-
a sensation of skipped beats or “pauses” in the heartbeat;
-
a weak, poorly palpable pulse.
Such disturbances are associated with damage to the heart muscle and increase the risk of dangerous arrhythmias during a heart attack.
Where the Pain Is Felt During a Heart Attack
Pain during a heart attack is not always limited to the area of the heart. Most often, it is localized behind the breastbone, but it can spread to other parts of the body.
Typical areas of pain radiation include:
-
the left arm or shoulder;
-
the neck and lower jaw;
-
the back, between the shoulder blades;
-
the upper abdomen.
In some cases, chest pain may be absent, and the main manifestations become shortness of breath, weakness, or discomfort in atypical areas, which makes timely recognition of a heart attack more difficult.
How the Heart Hurts During a Heart Attack
Pain during a heart attack has characteristic features. Most often, it is intense, pressing, squeezing, or burning. An important distinction is that such pain does not go away with rest and does not decrease after taking medications.
Painful sensations may increase gradually or occur suddenly. They are often accompanied by cold sweat, nausea, pronounced weakness, and a feeling of fear, which are typical manifestations of an acute heart attack.
What to Do During a Heart Attack
If a heart attack is suspected, action must be taken immediately. The extent of heart muscle damage and the risk of complications depend on the first minutes. Waiting it out or trying to “endure” the symptoms is dangerous.
The algorithm of actions in case of a suspected heart attack should be as follows:
-
immediately call emergency medical services;
-
stop any physical activity, sit down or lie down with the upper body elevated;
-
ensure access to fresh air, loosen tight clothing;
-
do not eat food or drink alcohol;
-
do not attempt to go to the hospital on your own.
Further actions depend on the patient’s condition and the results of examinations, in particular the electrocardiogram.
Does an ECG Show a Heart Attack
An electrocardiogram (ECG) is the main and fastest method for diagnosing a heart attack. In most cases, it allows detection of acute myocardial damage within the first minutes after the onset of an attack.
An ECG may show:
-
signs of an acute heart attack;
-
changes characteristic of cardiac ischemia;
-
heart rhythm disturbances;
-
consequences of a previous heart attack.
At the same time, in very early stages or in some forms of heart attack, the ECG may be insufficiently informative. In such situations, the diagnosis is уточified using repeated ECGs, blood tests for cardiac markers, and additional examinations.
What You Can Eat During a Heart Attack
Nutrition during a heart attack and the recovery period should be as gentle as possible for the heart and blood vessels. In the acute phase, only light food in small portions is usually allowed, and after stabilization of the condition, a special diet is formed.
Foods that are usually recommended after a heart attack include:
-
boiled or stewed vegetables;
-
light vegetable soups;
-
cereals cooked in water or low-fat milk;
-
lean fish;
-
boiled or baked lean meat;
-
low-fat fermented dairy products;
-
fruits in baked or pureed form.
At the same time, it is recommended to limit salt, fatty foods, fried dishes, sweets, and products high in cholesterol. Final dietary recommendations are always provided by a doctor, taking into account the patient’s condition.
How Long a Heart Attack Lasts
The duration of a heart attack can vary. In most cases, acute pain and the main symptoms of a heart attack last from 20–30 minutes to several hours. Unlike angina, pain during a heart attack does not resolve on its own and does not go away after taking nitroglycerin.
The acute phase of a heart attack usually lasts the first 24 hours, and it is during this period that the risk of complications is highest. Complete formation of the damaged area of the heart occurs over several weeks.
The earlier a patient receives medical care, the shorter the attack may be and the greater the chances of reducing the extent of myocardial damage and avoiding severe consequences.
How to Prevent a Heart Attack

Prevention is aimed at reducing the load on the heart and eliminating factors that lead to impaired blood supply to the myocardium. In most cases, a heart attack does not occur suddenly — it is preceded by long-term changes in blood vessels and heart function that can be detected and corrected.
The basis of prevention is regular monitoring of the cardiovascular system. Modern cardiology makes it possible to detect coronary heart disease, rhythm disturbances, hypertension, and other conditions that increase the risk of a heart attack at early stages. Routine check-ups are especially important for people over 40 years of age, as well as for patients with chronic diseases.
Key preventive measures include:
-
monitoring blood pressure and maintaining it within an individual normal range;
-
correcting cholesterol and blood glucose levels;
-
rational nutrition with limitation of salt, animal fats, and simple carbohydrates;
-
moderate regular physical activity agreed upon with a doctor;
-
quitting smoking and avoiding alcohol abuse;
-
reducing the impact of chronic stress and ensuring adequate sleep;
-
adherence to prescribed medication therapy, if recommended by a doctor.
Special attention to prevention should be given to people who have already experienced a heart attack or have diseases of the heart and blood vessels. In such cases, regular medical supervision and adherence to recommendations significantly reduce the risk of a recurrent heart attack.
Understanding individual risk factors and taking a responsible approach to health make it possible not only to reduce the likelihood of an attack but also to maintain quality of life for many years.