Contents:
- Why a pelvic ultrasound is performed
- Pelvic ultrasound: what is included in the diagnostics
- When is the best time to have a pelvic ultrasound
- How to prepare for a pelvic ultrasound
- What a pelvic ultrasound shows
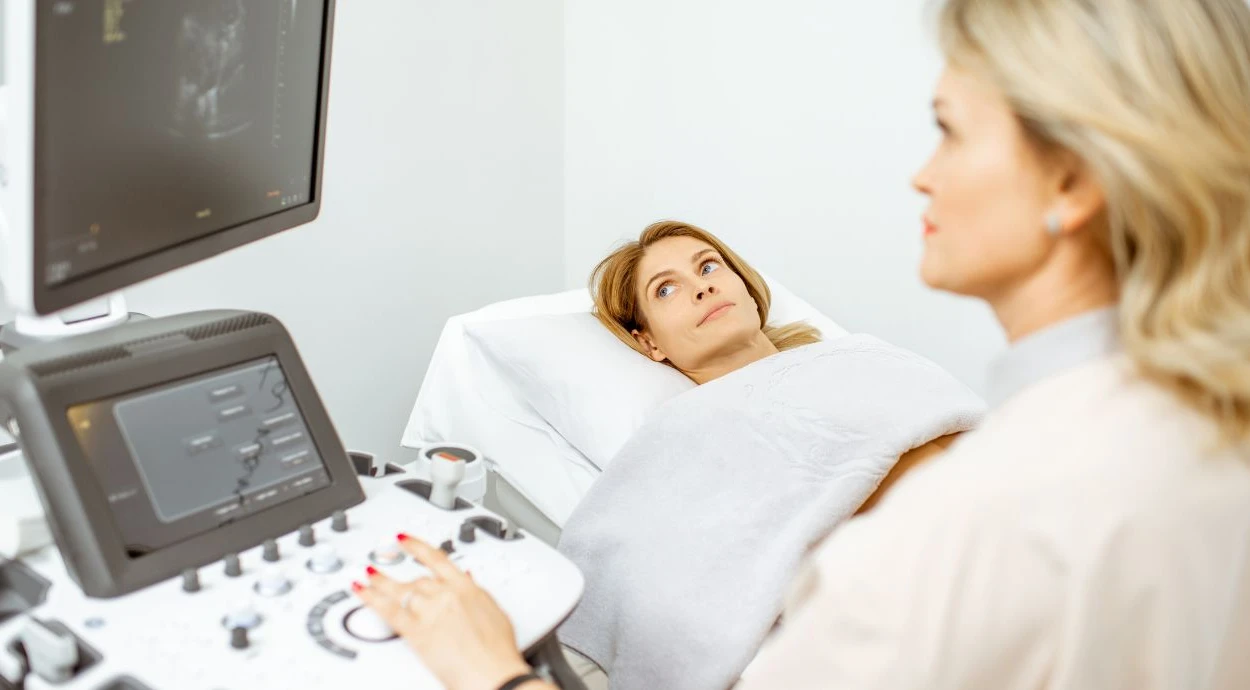
A pelvic ultrasound examination is prescribed for lower abdominal pain, menstrual cycle disorders, problems with conception, and for preventive monitoring of women’s health. The examination is painless, takes little time, and makes it possible to assess the condition of the uterus, ovaries, and endometrium.
However, the informative value of the examination largely depends on the correctly chosen timing and adherence to recommendations before the procedure. In this article, we will discuss on which day of the cycle to have a pelvic ultrasound and which simple rules will help you obtain an accurate result.
Why a pelvic ultrasound is performed
In gynecology, a pelvic ultrasound is prescribed both when there are complaints and for preventive purposes. This examination helps assess the condition of the internal organs, detect structural changes, and determine further examination or treatment tactics.
The most common indications for the examination are:
- lower abdominal pain, pulling or sharp sensations;
- menstrual cycle disorders — delays, overly heavy or scanty menstruation;
- intermenstrual spotting;
- suspected cysts, fibroids, polyps, or other neoplasms;
- difficulties with conception or preparation for pregnancy planning.
As part of a preventive examination, ultrasound diagnostics may be recommended even in the absence of complaints. Regular monitoring makes it possible to detect changes at an early stage, when they are not yet accompanied by symptoms.
After surgical interventions or a course of treatment, the examination is used to assess the dynamics of the condition and exclude complications.
Separately, ultrasound is used for folliculometry — monitoring follicle growth during pregnancy planning. In this case, the examination is performed on certain days of the cycle to assess the approach of ovulation.
After receiving the results, a gynecologist consultation is recommended. The doctor will explain the conclusion, correlate it with the clinical picture, and, if necessary, determine further steps. It is important to remember that an ultrasound conclusion is not an independent diagnosis and requires medical interpretation.
Pelvic ultrasound: what is included in the diagnostics
During the examination, the doctor assesses the anatomical structure, size, tissue structure, and relative position of the pelvic organs. The scope of the examination depends on the patient’s complaints, age, and the clinical task.
Standardly, during such an ultrasound, the following are assessed:
- the uterus — its size, shape, contours, and the condition of the myometrium;
- the endometrium — thickness and correspondence to the phase of the menstrual cycle;
- the cervix — structure and the presence of pathological changes;
- the ovaries — size, number of follicles, the presence of cysts or other formations;
- the space behind the uterus — the presence of free fluid;
- the bladder — as an overview, to exclude concomitant changes.
The examination is performed transabdominally (through the anterior abdominal wall) or transvaginally. The transvaginal method is more informative, as it makes it possible to examine the structure of the endometrium and ovaries in more detail. The choice of examination method depends on the clinical situation.
When is the best time to have a pelvic ultrasound
The day of the ultrasound depends on the purpose of the examination. Since the endometrium and ovaries change throughout the menstrual cycle, choosing the right time increases the informative value of the diagnostics.
Recommended timeframes:
- Day 5–7 of the cycle (immediately after menstruation) — for an overall assessment of the uterus and ovaries, detection of fibroids, polyps, cysts, and structural changes. During this period, the endometrium is thin, so pathological formations are better visualized.
- Day 8–10 of the cycle — to уточнення the condition of the endometrium if there is suspicion of hyperplasia or intrauterine neoplasms.
- Day 12–16 of the cycle — for folliculometry (monitoring follicle growth and the approach of ovulation). The examination may be performed several times during the cycle.
- Day 21–23 of the cycle (with a 28-day cycle) — to assess the second phase, the condition of the corpus luteum, and the thickness of the endometrium when planning pregnancy or if endometriosis is suspected.
- Any day of the cycle — in case of acute pain, suspected ectopic pregnancy, ovarian apoplexy, or other urgent conditions.
If the cycle is irregular, the day of the examination is determined individually. That is why the question of which day of the cycle to have a pelvic ultrasound is best уточнювати with a doctor, taking into account the specific clinical situation.
How to prepare for a pelvic ultrasound
Preparation depends on the method of the examination — transabdominal or transvaginal. Correctly following the recommendations helps obtain a clear image and avoid the need for a repeat examination.
For transabdominal ultrasound (through the anterior abdominal wall):
- about 1 hour before the procedure, drink approximately 500–800 ml of still water;
- do not empty the bladder before the examination.
A moderately filled bladder improves visualization of the uterus and ovaries.
For a transvaginal ultrasound, no special preparation is needed. For greater comfort, it is advisable to empty the bladder before the procedure.
Exact recommendations regarding what preparation for an ultrasound should be are to be provided by the doctor. It may differ slightly depending on the clinical situation.
What a pelvic ultrasound shows
Ultrasound makes it possible to detect structural changes in the uterus and ovaries, assess the condition of the endometrium, and determine the presence of pathological formations. The examination shows the size of the organs, their shape, the uniformity of tissues, and possible deviations from the norm.
During the examination, the following may be detected:
- • uterine fibroids;
• endometrial polyps;
• endometrial hyperplasia;
• ovarian cysts;
• signs of an inflammatory process;
• the presence of free fluid in the pelvis;
• space-occupying lesions of unclear nature.
Ultrasound also makes it possible to assess follicle growth and the fact of ovulation, determine the presence of the corpus luteum in the second phase of the cycle, and, in the early stages, confirm an intrauterine pregnancy.
It is important to understand that an ultrasound examination shows anatomical changes, but does not always make it possible to establish a final diagnosis. To determine it, the doctor considers clinical symptoms and the results of other examinations.
The information in this article is provided for informational purposes only and is not intended as a guide to self-diagnosis or treatment. If symptoms of the disease appear, consult a doctor.
Sources: