Contents:
- What is lichen: how it looks and how it is treated
- What is lichen
- How lichen begins
- What lichen looks like
- What types of lichen occur in humans
- How lichen is transmitted
- How to treat lichen
- How to understand that lichen is resolving
- When to see a doctor
What is lichen: how it looks and how it is treated
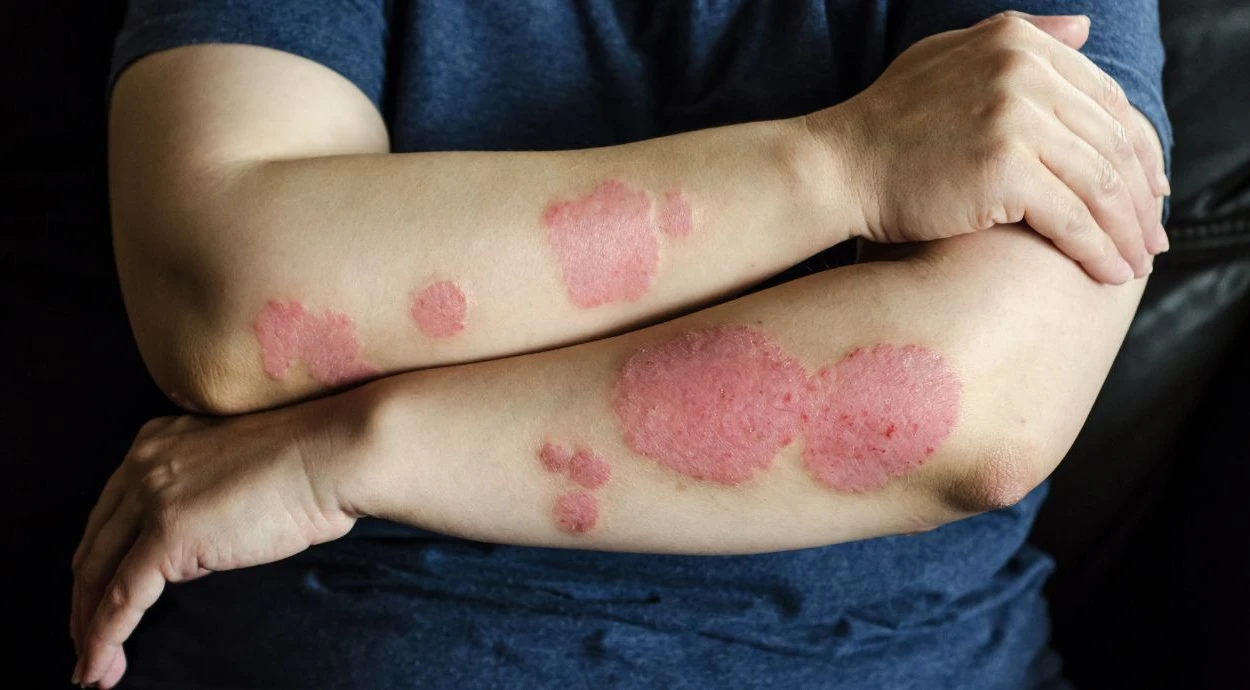
Round spots on the skin, redness with scaling, or rashes with well-defined edges may be manifestations of lichen. This is not a separate disease, but a generalized term for various dermatological conditions that differ in their causes and mechanisms of development.
Some forms have a fungal origin, others are associated with a viral infection or a reaction of the immune system. That is why it is important to correctly determine the type of lesion, since the therapeutic approach differs in each case.
In this article, we will consider what lichen is, how it looks, what types exist, how to treat lichen in humans, and when it is necessary to consult a doctor.
What is lichen
Lichen is a skin disease that occurs due to an infectious factor or a disorder of the immune system and is accompanied by an inflammatory reaction in the affected area.
In fungal infections, the pathogen multiplies in the upper layers of the skin and may affect hair follicles. Viral forms develop after infection or activation of the virus in the body. Inflammatory forms are associated with a disturbance of the immune response, when the body mistakenly perceives its own tissues as foreign.
The duration of the disease may vary: some forms are temporary and resolve on their own, while others may become chronic with periodic exacerbations.
How lichen begins
The onset of the disease may differ depending on its type; however, in most cases, the changes appear gradually. At first, the lesion may be barely noticeable and not accompanied by pronounced discomfort.
The most common early signs are:
- the appearance of a small spot or an area of skin discoloration;
- gradual enlargement of this area;
- mild itching or a burning sensation;
- dryness or slight scaling;
- increased sensitivity or tingling in the affected area.
In some cases, one larger element appears first, and later additional rashes develop. In certain forms, general malaise may occur before skin changes appear.
At the initial stage, it is not advisable to use aggressive ointments or antiseptics on your own, as this may alter the manifestations of the disease and complicate the establishment of an accurate diagnosis.
What lichen looks like
The external appearance of the lesion depends on the type of disease. Most often, these are limited areas of altered skin with well-defined or slightly blurred edges. The color may vary from pink and red to brown or lighter than the surrounding skin.
For certain forms, the following signs are characteristic:
- round or oval spots of various sizes;
- scaling in the center or along the edges;
- the appearance of small fluid-filled blisters;
- formation of crusts after the elements dry;
- dense nodules or plaques;
- hair loss in the affected area (when the scalp is involved).
In the viral type, the rash may be located on one side of the body and be accompanied by pain along the nerve endings. In fungal infections, a clearly defined ring-shaped outline with a lighter center is often noticeable. It is the combination of these signs that allows the doctor to suspect a specific type of disease and determine further examination tactics to establish an accurate diagnosis.
.jpg)
What types of lichen occur in humans
In humans, several forms of lichen are most commonly diagnosed, differing in their cause and mechanism of development. Accurate determination of the type is of fundamental importance, since the therapy differs in each case.
Pink lichen
Pink lichen (Gibert’s disease) usually occurs after a viral infection or against the background of reduced immunity. First, one larger spot appears, after which smaller elements develop on the trunk within several days or weeks.
The condition is benign and in most cases resolves on its own. The disease is not considered contagious. Treatment is aimed at reducing itching and inflammation.
Ringworm
Ringworm is a fungal infection of the skin or scalp. When hair is affected, it becomes brittle and may fall out within the lesion. Infection occurs through contact with an infected person, animal, or household items. The infection may spread without treatment; therefore, mandatory antifungal therapy is required.
Shingles
Shingles is caused by the varicella-zoster virus — the same virus that causes chickenpox. After a person has had chickenpox, the virus remains in the nerve cells and may reactivate when immunity decreases.
The rash is located on one side of the body along the course of a nerve and is accompanied by pain, burning, or increased sensitivity. Treatment is aimed at suppressing viral activity and reducing pain.
Pityriasis (tinea versicolor)
This is a superficial fungal infection of the skin caused by yeast-like fungi of the genus Malassezia. It manifests as spots of various shades — from light to brown. It is more often localized on the back, chest, and shoulders. The disease may recur, especially in warm seasons or with increased sweating.
Lichen planus
Lichen planus has an inflammatory nature and is associated with impaired immune regulation. Dense, shiny nodules appear on the skin and may be accompanied by itching. The process may affect not only the skin but also the mucous membrane of the oral cavity. The disease is not contagious and may have a prolonged course; therefore, medical supervision is required.
How lichen is transmitted
The mechanism of transmission depends on the type of disease. Not all forms of lichen are contagious; therefore, the risk of infection is determined by the specific cause of the lesion.
Fungal forms may be transmitted:
- through close contact with an infected person;
- via shared towels, combs, hats, or bed linen;
- through contact with infected animals;
- in public places with high humidity (swimming pools, gyms).
Shingles is not transmitted as classic “lichen”; however, a person with active lesions may infect those who have not had chickenpox, causing chickenpox in them. Pink lichen and lichen planus are not considered contagious and are not transmitted through household contact.
To reduce the risk of fungal infection, it is important to maintain personal hygiene, use individual care items, and avoid contact with stray animals.
How to treat lichen
The treatment strategy depends on the type of disease, the localization of the lesion, the extent of skin changes, and the general condition of the patient. There is no single medication suitable for all forms. Therefore, before starting treatment, it is important to establish the exact cause of the lesion.
To determine how to get rid of lichen, the doctor performs a skin examination and, if necessary, prescribes additional tests. In particular, dermatoscopy may be used — a method of examining the skin under magnification, which allows detailed assessment of the structure of the lesion and clarification of its nature.
Depending on the established diagnosis, different groups of medications are used.
| Group of medications | When they are used | Examples of active substances |
| Antifungal agents | For fungal forms (ringworm, pityriasis) | terbinafine, ketoconazole, clotrimazole, fluconazole |
| Antiviral medications | For shingles | acyclovir, valacyclovir, famciclovir |
| Anti-inflammatory agents | For pronounced inflammation or itching | topical glucocorticosteroids |
| Antihistamines | To reduce itching | cetirizine, loratadine |
| Antiseptic agents | For prevention of secondary infection | chlorhexidine, drying solutions |
In fungal forms, topical creams, ointments, or solutions are usually used. If the lesion is extensive or the scalp is involved, the doctor may prescribe systemic antifungal medications in tablet form. The duration of therapy is determined individually and may last several weeks.
In shingles, treatment should be started as early as possible. Antiviral medications are prescribed, as well as drugs to reduce pain. In some cases, additional therapy is required to prevent complications affecting the nervous system.
Pink lichen in most cases does not require specific drug therapy. Gentle skin care and agents to reduce itching are recommended. Lichen planus is treated with medications that reduce the inflammatory response.
How to understand that lichen is resolving
Signs of recovery depend on the type of disease; however, there are general criteria indicating positive dynamics. First of all, the intensity of inflammation decreases: redness becomes less pronounced, and the borders of the lesion gradually lose their clarity. Itching and burning weaken or disappear completely. In fungal forms, enlargement of the lesion stops and no new elements appear.
For shingles, drying of the blisters with subsequent crust formation is characteristic; the crusts gradually fall off. In pityriasis, the spots may persist for some time, but without active scaling or spreading — this indicates completion of the infectious process.
It is important to remember that residual skin discoloration may persist even after complete recovery. This does not always mean that the disease is ongoing. The effectiveness of therapy should be evaluated by a doctor, especially if lichen treatment is carried out with systemic medications.
When to see a doctor
A consultation with a dermatologist is necessary in cases when:
- the rash rapidly increases or spreads to new areas;
- pronounced pain, swelling, or oozing appears;
- the scalp is affected;
- symptoms do not decrease within several days;
- the rash occurs in a child, an elderly person, or a patient with weakened immunity.
Shingles require immediate medical attention, especially if the rash is localized on the face or is accompanied by severe pain.
Self-treatment without establishing the exact type of disease may lead to complications or progression to a chronic form. Timely diagnosis allows the selection of effective and safe therapy.
The information in this article is provided for informational purposes only and is not intended as a guide to self-diagnosis or treatment. If symptoms of the disease appear, consult a doctor.
Sources:
PubMed — National Library of Medicine (StatPearls): Pityriasis Rosea
PubMed — National Library of Medicine (StatPearls): Lichen Planus
PubMed — National Library of Medicine: Pityriasis Rosea: Diagnosis and Treatment