Contents:
- What Is a Trophic Ulcer
- How a Trophic Ulcer Begins
- What a Trophic Ulcer Looks Like and Why It Is Dangerous
- How to Treat Trophic Ulcers
- What Is the Best Way to Treat Trophic Ulcers
- How to Prevent the Development of the Disease
A trophic ulcer does not appear suddenly: it usually forms against the background of long-term circulatory disorders. It may be preceded by swelling, changes in skin color, itching, tissue thickening, or small injuries that do not heal for a long time. Most often, such lesions occur on the lower legs and require not only local treatment, but also identifying the underlying cause.
Self-care may temporarily reduce discomfort, but it does not eliminate the problem if venous or arterial blood flow is impaired. In this article, we will discuss how a trophic ulcer begins, which symptoms should not be ignored, what can be used to safely rinse the affected area, and why treatment must be comprehensive.
What Is a Trophic Ulcer
A trophic ulcer is an open area of skin damage that does not heal for a long time due to impaired blood circulation. Most often, it occurs on the lower leg or near the ankle. Its development may be associated with varicose vein disease, chronic venous insufficiency, worsening arterial blood flow, or complications of diabetes mellitus.
Unlike a common superficial injury, a trophic ulcer does not close within a few days. It may remain open for weeks, ooze, hurt, increase in size, or reopen after temporary improvement.
The main problem is not only skin damage. When venous outflow is impaired or arterial blood reaches the tissues in insufficient amounts, healing slows down. Because of this, even a small scratch, shoe-related abrasion, or skin crack can turn into a chronic wound.
Doctors at Oxford Medical warn: a trophic ulcer should not be considered only a superficial defect that can simply be covered with ointment or a dressing. It is important to find out why it appeared, assess the condition of the blood vessels, and choose care that will not harm the wound and will help create conditions for healing.
How a Trophic Ulcer Begins
A trophic ulcer rarely appears immediately as a deep wound. Most often, symptoms that indicate impaired blood circulation in the leg appear first: swelling, heaviness, itching, burning, or a change in skin color in the lower part of the lower leg. In many people, these symptoms worsen after standing for a long time or by the end of the day.
Over time, the skin becomes more sensitive and vulnerable to injury. It may peel, thicken, become easily injured, or heal slowly even after a minor scratch or rubbing from footwear. If the circulatory disorder progresses, a wound that does not close for a long time may form at the site of such injury.
Conditions that worsen venous outflow or blood supply to tissues may lead to the development of a trophic ulcer. In particular, previous deep vein thrombosis can cause chronic circulatory impairment in the lower limb. In such cases, the risk of swelling, skin changes, and non-healing wounds increases significantly.
The first signs to pay attention to are:
- regular swelling of the lower leg or foot;
- darkening, redness, or a bluish skin tone;
- itching, burning, or a feeling of tightness;
- thickening of the skin in the lower leg area;
- the appearance of a crack, oozing area, or small wound;
- skin damage that does not heal within 1–2 weeks.
Doctors at Oxford Medical recommend not ignoring even minor skin changes on the legs if they are combined with swelling or varicose veins. The earlier the cause of impaired blood circulation is identified, the higher the chances of preventing the formation of a trophic ulcer.
What a Trophic Ulcer Looks Like and Why It Is Dangerous
.jpg)
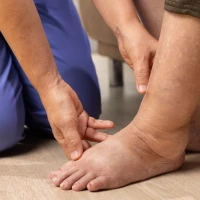
A trophic ulcer looks like a wound on the skin that does not heal for a long time. At first, it may be a small area of skin damage, but over time the wound increases in size, begins to ooze, and the color and structure of the skin around it change.
The affected area may be red, dark brown, or bluish. The surrounding skin often becomes denser, dry, shiny, and sensitive to touch. Plaque or crusts sometimes appear on the surface of the ulcer. In some cases, pain, burning, itching, or an unpleasant odor may occur.
As shown by a study published in the international scientific database PubMed, chronic venous ulcers have a high risk of infection and may remain unhealed for a long time without comprehensive treatment.
The danger of a trophic ulcer is that an open wound is easily infected and may gradually increase in size. Without proper treatment, inflammation can spread to the surrounding tissues, and the healing process may last for months.
How to Treat Trophic Ulcers
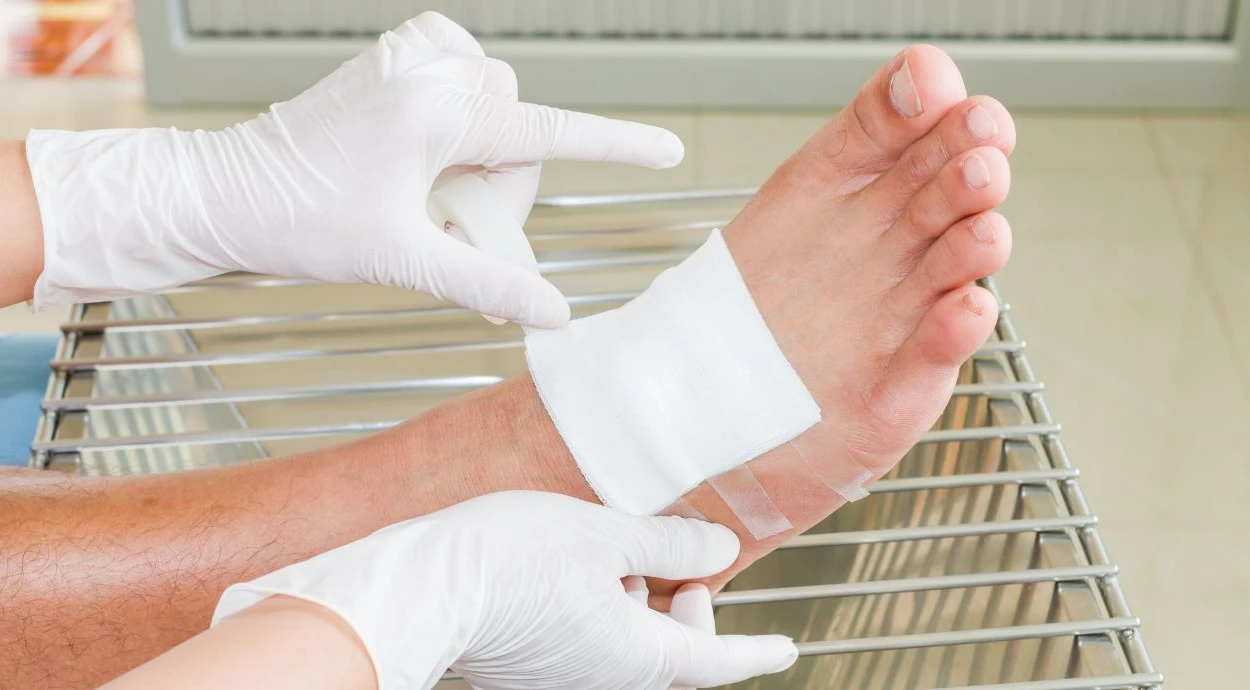
A trophic ulcer should be treated carefully so as not to injure the tissues or introduce infection. Before changing the dressing, it is necessary to wash your hands, prepare sterile wipes, a rinsing solution, and a clean dressing.
The old dressing must not be torn off with sudden movements. If it has dried onto the wound, it should be moistened with saline solution and left for a few minutes. This helps avoid tissue damage and bleeding.
After cleansing, the wound is covered with a sterile dressing. It should not press too tightly, but it should protect the ulcer from contamination and friction from clothing or footwear. The dressing should be changed as often as recommended by the doctor, or earlier if it becomes heavily soaked or contaminated.
During care for a trophic ulcer, it is important to:
- avoid touching the wound with dirty hands;
- avoid using cotton wool inside the ulcer;
- avoid covering the wound with a regular plaster without air access;
- avoid removing crusts and plaque on your own;
- monitor for pus, a sharp odor, or increased redness.
Our doctors recommend consulting a specialist if the wound increases in size, starts to hurt more, or pronounced swelling appears around it. Such symptoms may indicate infection or worsening blood circulation.
What to Rinse Trophic Ulcers With
For rinsing trophic ulcers, sterile 0.9% sodium chloride saline solution is most often used. It is suitable for regular wound cleansing, helps remove discharge, and does not irritate the tissues.
After removing the dressing, the ulcer is gently rinsed with saline using a sterile wipe or a syringe without a needle. There is no need to rub the wound surface strongly — cleansing should be gentle.
If there is plaque or dried discharge on the surface, it must not be torn off. First, the area should be moistened with the solution for a few minutes so that the tissues soften and clean without additional trauma.
In some cases, the doctor may recommend special products for cleansing chronic wounds — for example, solutions based on octenidine or polyhexanide. They are used when there is an increased risk of infection or if the wound is poorly cleansed with ordinary saline.
Doctors at Oxford Medical warn: for regular care of trophic ulcers, it is not recommended to use alcohol, concentrated iodine, brilliant green, or frequently treat the wound with hydrogen peroxide, because such products may dry out tissues and irritate the surface of the ulcer.
How to Relieve Pain from Trophic Ulcers
.jpg)
Pain from trophic ulcers occurs due to tissue inflammation, swelling, irritation of nerve endings, and impaired blood circulation. In some people, discomfort is moderate, but sometimes the pain becomes so severe that it interferes with normal walking and sleep.
To reduce pain, the doctor may recommend pain-relieving medicines — most often based on paracetamol or nonsteroidal anti-inflammatory drugs. If the ulcer is infected or there is pronounced inflammation around it, pain may also gradually decrease after treatment of the infection begins.
In venous trophic ulcers, discomfort often worsens due to swelling and blood stagnation in the legs. In such cases, the doctor may recommend compression therapy — elastic bandages or compression hosiery. This helps improve venous outflow, reduce swelling, and relieve pain. However, in cases of severe arterial blood flow impairment, compression is not suitable for everyone, so it is used only after vascular examination.
To reduce pain, it is also important to:
- avoid overloading the legs by standing for a long time;
- slightly elevate the legs during rest;
- wear soft, comfortable shoes that do not rub the skin;
- change dressings regularly, preventing them from drying out;
- avoid injuring the ulcer area.
Doctors at Oxford Medical recommend not tolerating severe or persistent pain from a trophic ulcer. If the discomfort suddenly worsens, pulsation, heat, or redness around the wound appears, this may indicate infection or worsening blood circulation and requires a medical examination.
What Is the Best Way to Treat Trophic Ulcers
Effective treatment of trophic ulcers on the legs is impossible without eliminating the cause of impaired blood circulation. If treatment is limited only to ointments or dressings, the wound may temporarily decrease in size, but the risk of recurrence will remain high.
As stated in the NCBI Bookshelf review on the treatment of chronic venous ulcers, the standard approach includes compression therapy, wound cleansing, modern dressings, antimicrobial treatment when indicated, and, if necessary, correction of venous blood flow.
The treatment strategy depends on what exactly caused the ulcer: varicose vein disease, venous insufficiency, diabetes mellitus, impaired arterial blood flow, or a combination of several causes.
For trophic ulcers associated with venous stasis, it is important to reduce swelling and improve venous outflow. For this purpose, the following may be used:
- compression hosiery or elastic bandaging;
- medications to support venous circulation;
- regular dressings;
- controlled physical activity;
- management of lower limb swelling.
If a non-healing wound developed against the background of varicose vein disease, the doctor may recommend vein treatment. In modern phlebology, minimally invasive methods are used for this, in particular EVLT, which helps eliminate pathological venous blood flow and reduce the risk of formation or recurrence of trophic ulcers.
If there are signs of infection, antibacterial medicines may be prescribed, and if there is a large amount of dead tissue, professional wound cleansing may be performed. In some cases, modern dressings are used to maintain a moist environment and support healing.
Our doctors recommend not trying to treat a trophic ulcer independently with home remedies alone. Chronic wounds require assessment of the vascular condition, control of concomitant diseases, and properly selected care. In most cases, the necessary care is provided by a vascular surgeon, because impaired blood circulation is most often the main cause of trophic ulcer formation.
How to Prevent the Development of the Disease
Prevention is primarily aimed at controlling diseases that impair blood circulation in the legs. Most often, these are varicose vein disease, chronic venous insufficiency, diabetes mellitus, and the consequences of vascular diseases.
To reduce the risk of trophic ulcers, it is important to:
- not ignore persistent swelling, heaviness, or pain in the legs;
- treat varicose vein disease in a timely manner;
- control blood sugar levels in diabetes;
- avoid prolonged standing or sitting without movement;
- wear comfortable shoes that do not rub the skin;
- care for the skin of the lower legs and feet, preventing cracks and injuries;
- follow the doctor’s recommendations on using compression hosiery.
People with varicose vein disease should be regularly monitored by a specialist, even if the symptoms seem minor. Timely treatment of venous circulatory disorders helps reduce the risk of chronic wounds in the future.
As noted in the National Health Service (NHS) recommendations, control of venous insufficiency, physical activity, and proper skin care help reduce the risk of developing venous ulcers.
A trophic ulcer is a chronic wound that requires not only local care, but also treatment of the cause of impaired blood circulation. The earlier a person pays attention to swelling, skin changes, or wounds that do not heal for a long time, the higher the chances of avoiding complications and prolonged treatment.
The information in this article is provided for informational purposes and is not an instruction for self-diagnosis or self-treatment. If symptoms of the disease appear, you should consult a doctor.
Sources: