A bivalent vaccine that provides protection against types 16 and 18 of the human papillomavirus. These types are most often associated with the development of cervical cancer. For girls under the age of 14, a schedule of two vaccine doses with a certain interval between injections is usually used. The vaccine forms a stable immune response and is widely used in cancer prevention programs.
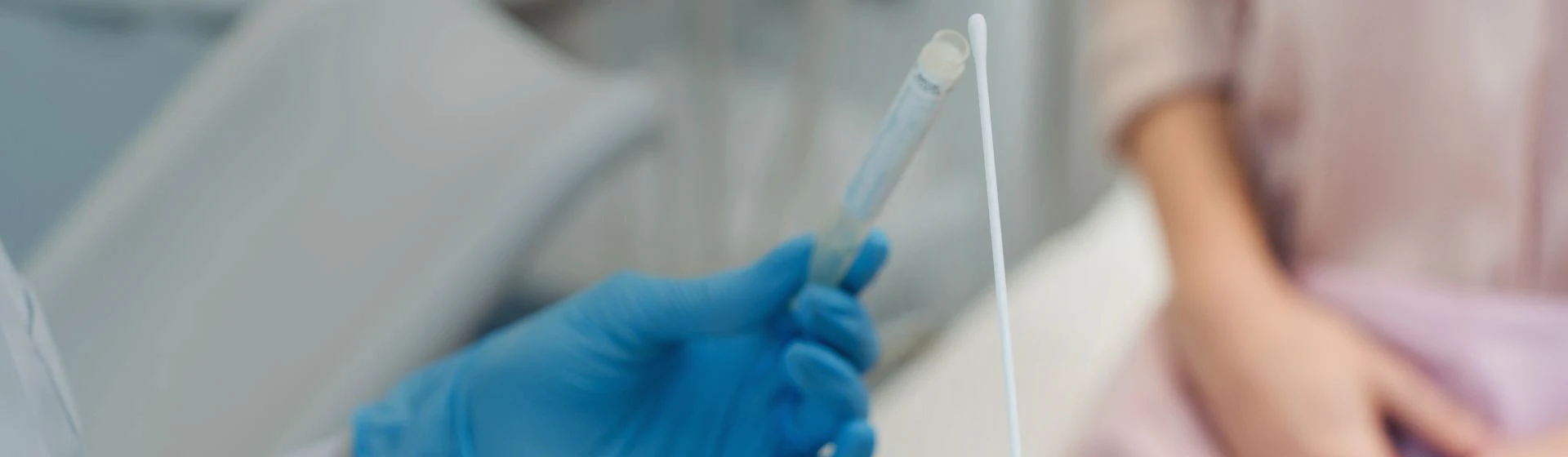
Human Papillomavirus (HPV) Vaccination
Human papillomavirus is one of the most widespread infections in the world. Most people become infected with it during their lifetime, often not even suspecting it. Certain types of the virus can lead to the development of cervical cancer, anal canal cancer, oropharyngeal cancer, as well as the appearance of genital warts. That is why vaccination against human papillomavirus is today recognized as the most effective method of prevention of oncogenic types of HPV.
Types of vaccines against human papillomavirus
Modern vaccines are used to prevent infection with the human papillomavirus, forming immunity against the most dangerous types of HPV. They do not contain a live virus and therefore cannot cause infection. After administration, the vaccine stimulates the production of antibodies that help the body recognize and neutralize the virus before it enters the cells.
Today, several types of vaccines are used for the prevention of HPV, differing in the number of virus types against which immune protection is formed.
Cervarix
Gardasil
A quadrivalent vaccine that provides protection against four types of HPV — 6, 11, 16, and 18. Types 16 and 18 are associated with the development of oncological diseases, while types 6 and 11 most often cause genital warts (condyloma acuminata). Due to this combination, the vaccine helps reduce the risk of both precancerous changes and clinical manifestations of the infection.
Gardasil 9
A nine-valent vaccine that provides the broadest spectrum of protection. It forms immunity against nine types of the human papillomavirus: 6, 11, 16, 18, 31, 33, 45, 52, and 58. These types are most often associated with the development of precancerous changes and oncological diseases. Due to its extended composition, the vaccine significantly reduces the risk of cervical cancer and other HPV-associated pathologies.
*The list and availability of vaccines are subject to change. Please check for the latest information when booking.
Modern HPV vaccines do not contain a live virus. They cannot cause infection or provoke symptoms of HPV in women. After administration, the papillomavirus vaccine stimulates the body to produce antibodies that block the virus before it can enter the cells.
Indications for the use of the papillomavirus vaccine
Vaccination against papillomavirus is also recommended for young women aged 15 to 26 years, and according to individual indications may be used in women up to 45 years of age. Even after the onset of sexual activity, vaccination remains advisable, as the vaccine provides protection against various types of human papillomavirus.
The papillomavirus vaccine does not treat an existing infection. If infection has already occurred, the virus may remain asymptomatic for a long time or manifest clinically. Among the possible manifestations are changes in cervical cells detected during screening, or the appearance of genital warts in the area of the external genital organs. In such cases, removal of genital warts on the genital organs by modern minimally invasive methods is possible. The procedure eliminates the external manifestations of the infection; however, it does not replace prevention and further medical supervision.
Separately, it should be noted that the HPV vaccine for women is an effective method of prevention and an important component of preserving reproductive health.
Contraindications and precautions for vaccination against papillomavirus
The HPV vaccine has a high safety profile and is well tolerated by most patients. However, there are situations when administration of the drug requires postponement or is not recommended.
Absolute contraindications are:
- anaphylactic reaction to a previous dose;
- confirmed hypersensitivity to the components of the drug.
Temporary postponement is possible in the case of an acute infectious disease with elevated temperature and pronounced deterioration of the general condition. Mild cold symptoms without fever usually are not grounds for refusal of vaccination; however, the final decision is made by the doctor after examination.
During pregnancy, administration of the vaccine is not carried out. If pregnancy occurs after the first dose, subsequent injections are postponed to the postpartum period. Breastfeeding is not a contraindication.
Before vaccination, examination by a gynecologist is mandatory. The doctor collects medical history, evaluates the state of health, and determines individual indications and possible risks.
Dose and administration of the human papillomavirus vaccine
The HPV vaccination schedule depends on the patient’s age, the type of vaccine, and the doctor’s recommendations. The earlier the vaccination is carried out, the more effectively immune protection is formed, since the body has not yet come into contact with the virus.
According to the updated National Immunization Schedule of Ukraine, from 2026 the HPV vaccine is recommended for girls aged 12–13 years. At this age, a two-dose vaccination schedule is usually used.
The following administration schedules are most commonly used:
- 9–14 years — 2 doses. The first dose is administered on the chosen day, the second — after 6 months. This schedule is used for the Cervarix or Gardasil 9 vaccines and allows a sufficient level of immune protection to be formed.
- from 15 years — 3 doses. The first injection is given on the designated day, the second — after 1–2 months, and the third — 6 months after the first.
The vaccine is administered intramuscularly in the shoulder area. The procedure takes only a few minutes and does not require special preparation. After the injection, the patient is recommended to remain under the supervision of medical staff for 15–20 minutes, which is a standard safety practice for any vaccinations.
If for certain reasons the intervals between doses were violated, the vaccination course usually does not need to be started again. The doctor will adjust the administration schedule and help complete the vaccination correctly.
Possible side effects of the HPV vaccine
The vaccine has a high level of safety and is well tolerated by most patients. Adverse reactions, if they occur, are usually mild and short-term.
The most frequently observed are:
- pain, redness, or slight swelling at the injection site;
- a feeling of weakness or a slight increase in temperature;
- headache.
Less often, dizziness, nausea, or short-term deterioration of well-being may occur. Such manifestations resolve on their own within 1–3 days and do not require special treatment.
Severe allergic reactions occur extremely rarely. That is why after administration of the vaccine, the patient remains under medical supervision for at least 15–20 minutes.
It is important to understand: the risk of developing serious complications from HPV significantly exceeds the likelihood of adverse reactions after vaccination. That is why preventive vaccination is considered a safe and justified method of protection.
Result of HPV vaccination
Immunity is maintained for 10–12 years. The most common side effect is temporary discomfort and redness at the injection site.
Vaccination against human papillomavirus ensures the formation of immunity by creating protective antibodies before infection with the virus. However, the vaccine will not protect if a woman is already infected with HPV. It is important to receive the vaccination before the onset of sexual activity, which increases the risk of infection.
How much does the HPV vaccine cost in Kyiv at the private clinic “Oxford Medical”
Vaccination against papillomavirus, the price of which depends on the selected preparation and the number of required doses, is carried out according to an individual scheme. The full course consists of two or three injections — this is determined by the age of the patient and the recommended administration schedule.
You can предварительно узнать the price of the HPV vaccine at the “Oxford Medical” clinic in Kyiv here. The doctor will provide more detailed information about the vaccination scheme and the final cost during the consultation.
At the “Oxford Medical” medical center, vaccination can be received not only in Kyiv but also in other cities of Ukraine. Our branches operate in most regions.
Make an appointment for a consultation at a time convenient for you — by phone or through the online chat on the website. The doctor will answer all your questions and select the optimal vaccination scheme specifically for you.
Frequently Asked Questions:
Where can I get the HPV vaccine in Kyiv?
You can get the HPV vaccine in Kyiv at the Oxford Medical medical center. Before vaccination, the doctor conducts a consultation, assesses your health, and determines the optimal administration schedule. Vaccination is carried out using certified drugs and in compliance with safety standards.
Which HPV vaccine is best?
The choice of vaccine depends on the patient’s age and the doctor’s recommendations. Today, several vaccines are used for the prevention of HPV. The Cervarix vaccine forms immunity against types 16 and 18, which most often cause cervical cancer. Gardasil provides protection against four types of the virus — 6, 11, 16, and 18. The broadest spectrum is provided by Gardasil 9, which forms immunity against nine types of HPV. The optimal vaccine and vaccination schedule are selected by the doctor individually after consultation.
Up to what age is HPV vaccination recommended?
The optimal age for vaccination is 9–14 years, before the onset of sexual activity. Vaccination is also recommended for young women up to 26 years of age, and may be given up to 45 years of age on an individual basis.
Is it necessary to get the HPV vaccine?
Vaccination is not mandatory, but it is recommended as an effective method of preventing precancerous changes and cervical cancer. The decision should be made individually after consulting with a doctor, taking into account age, medical history, and risk factors.
Can you get the HPV vaccine if you are already infected?
Yes, vaccination is possible even after contact with the virus. It does not cure an existing infection, but it helps to build protection against other types of HPV that the body has not yet been exposed to and reduces the risk of complications in the future.
How long does the HPV vaccine last?
After completing the full course, long-term immunity is formed. Studies confirm that protection lasts for more than 10–12 years. Currently, there is no need for routine revaccination if the schedule was completed according to the recommendations.
Our doctors


Specialist in aesthetic gynecology.





Let's take care
about your health:






